|
12/23/2023 0 Comments Sentinel node biopsy breast cancer Most patients resume regular activities within a few days and incisions generally heal within a few weeks. easier for the patient in terms of recuperation.A negative sentinel lymph node indicates a greater than 95 percent chance that the remaining lymph nodes are also cancer-free more accurate than the traditional axillary dissection in assessing whether breast cancer has spread to the lymph nodes.highly reliable in detecting cancerous cells.In less than five percent of sentinel node biopsies, the sentinel node cannot be identified and a full axillary dissection is done. Only the lymph nodes that have absorbed the radiotracer are removed. The surgeon makes an incision underneath the arm and passes a hand-held probe over the area to measure levels of radioactivity. Images may be taken to help the surgeon visualize the radiotracer’s ’s pathway as it leaves the breast. Prior to surgery to remove part of or the entire breast, a tiny amount of radioactive particles are injected in the area of the breast where the tumor is or around the nipple. In a sentinel node biopsy, only the sentinel nodes are surgically removed, which results in fewer complications and side effects for the patient, including lymphedema. Sentinel nodes collect the fluid draining from the tumor and are most likely to contain cancer cells if the tumor has metastasized, or spread. Molecular imaging is used to identify the first few, or sentinel, nodes into which a tumor drains. Because many sentinel node biopsies are followed by complete axillary dissections, the usefulness of the ability to more exhaustively evaluate the sentinel node for micrometastases may require further study.-r.s.A sentinel node biopsy is an established alternative to axillary lymph node dissection. They conclude that the question of whether sentinel node lymphadenectomy will eliminate elective axillary dissection should not be determined by the difference in morbidity rates. They noted minimal lymphedema, no range-of-motion difficulties, no prolonged pain, minimal numbness or parasthesias, and no recurrent disease in the axilla. 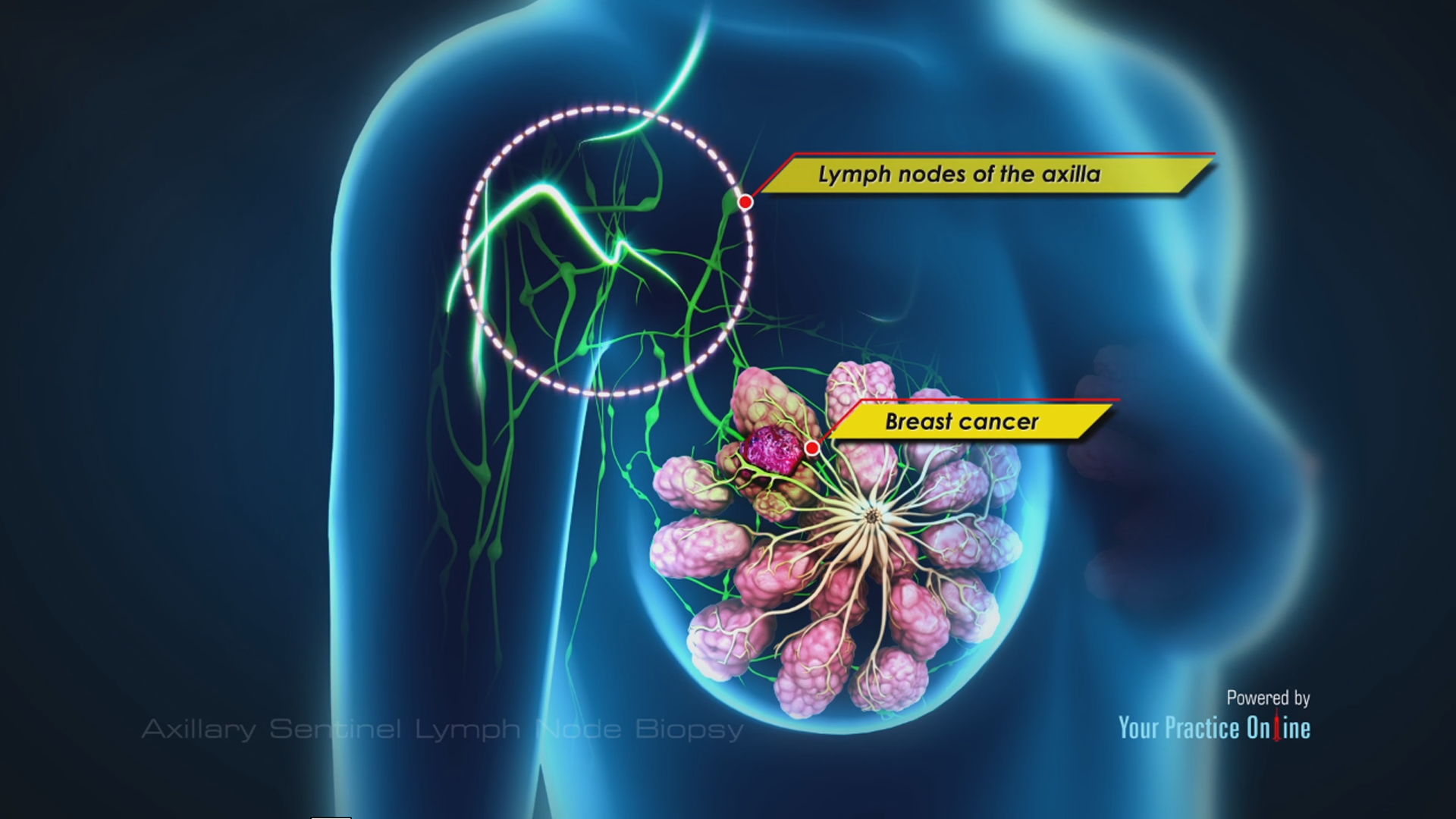
Complications of level I and II axillary dissection in the treatment of carcinoma of the breast. Roses and associates studied a series of patients who received level I and II node dissections ( Roses DF, et al. 
Another option is level I and level II axillary node dissection with preservation of the pectoralis minor the incidence of level III micrometastases without abnormalities at the two lower levels is rare. One of the supporting arguments for sentinel node surgery is that full axillary node dissection causes significant complications. Sentinel lymph node biopsy (SLNB) was first introduced as a technique of axillary nodal staging for breast cancer by Giuliano and Krag in 19 2,3. The guideline also recommends that sentinel lymph node biopsy should be offered to people who are having a mastectomy for ductal carcinoma in-situ breast cancer. Sentinel node biopsy of breast cancer is becoming an increasingly popular topic. Sentinel lymph node biopsy (SLNB) at upfront surgery is the gold-standard surgical method for axillary lymph node staging in early stage breast cancer: the technique provides adequate information regarding axillary status, with similar oncological safety and lower morbidity compared to axillary dissection, despite the false negative rates. The use of sentinel lymphadenectomy to identify micrometastases is becoming more popular, even though regional nodal dissection is recognized as useful in controlling nodal disease. Although node metastases aid in prognosis determination, the use of adjuvant systemic therapy makes this information less important for therapeutic decisions. Editor's note: The role of axillary dissection in the treatment of invasive breast cancer is being re-evaluated. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
